Burnout in Healthcare: Does It Really Exist?
People leading mental health and well-being can suffer from a lack of it. Read more to find out all about how we can build a more mentally fit workforce, especially in critical environments such a healthcare.
What is Burnout?
Burnout as a concept was introduced by the American psychoanalyst Herbert Freudenberger. He initially associated the term with the workplace stress experienced mainly by healthcare professionals like physicians, nurses, and pharmacists (1).
However, it is not restricted to these professions and could theoretically affect any chronically distressed employee who feels like he or she can’t keep up with their job’s or life’s demands.
Recently, in 2019, the world health organization (WHO) elaborated on the definition of burnout and referred to it as an occupational phenomenon that is bound to one’s experience in the workplace environment (2).
While the definition of burnout is vague, and there is debate as to whether the phenomenon really exists, most of us, at some point in our lives, have experienced the symptoms of burnout. From a resilience perspective, this is when we either suffer, bounce or grow. Some people report experiencing burnout in non-work aspects of life such as parenthood, friendships, romantic relationships, and caretaking.
How do I know If I am Burned Out?
Experts themselves can’t seem to agree on what or how common burnout actually is. However, there are symptoms and risk factors, which we explore below.

Symptoms
In general, Burnout is manifested by three main characteristics: negativism and cynicism, emotional exhaustion, and a decrease in professional productivity.
Needless to say, these features are often accompanied by mental and physical health complications, such as:
- Heartburn and gastrointestinal symptoms
- Headaches and fatigue
- Potential food, alcohol, and drug abuse.
Recognizing these signals is a step closer to better identifying whether or not work stress is negatively impacting your way of life.
Risk Factors (3)
The interplay between several environmental factors in an individual’s life and their psychological state contributes to the risk of them developing burnout in the workplace. Some of these risk factors include:
Lack of Control and Job Autonomy
The less flexibility an employee has in making workplace-related decisions, the more stressful the environment becomes. For example, a person dealing with emergency situations, especially in the healthcare sector, has limited control over work hours, schedules, tasks, and assignments.
This may increase feelings of helplessness and despondency in the worker.
High Job Demands
The mental health of any employee is most affected when combining negative emotions with an unmanageable workload or psychologically unsafe environment.
High-demanding jobs, whether long working hours or intensive and laborious tasks, put a lot of pressure on the employee. Without balancing performance with care (see the 2022 Global Report), these individuals are most likely living in a consistent state of anxiety and fatigue and are at higher risks of experiencing a downward spiral.
Lack of Moral Support
Many burned-out workers report a lack of connection or support.
A healthy work environment is one where colleagues, supervisors, and managers offer safe connection opportunities. If lacking, individuals might feel disconnected, isolated and vulnerable, all of which contribute to increased burnout risk.
Personality Traits
People with specific personality features tend to be more susceptible to burnout. A study of 298 Indian nurses suggests that neuroticism increases vulnerability to stress and burnout. Depression and post-traumatic stress disorders have also been revealed as burnout precursors.
Have the number of Burnt out Healthcare Workers changed over the past decade?
The number of healthcare professionals suffering from burnout is rising in all relevant sectors. The levels of clinicians, nurses, and paramedics who are suffering from exhaustion, depression, and anxiety have reached “crisis levels”.
As indicated by the 2019 National Academies of Medicine report, up to 60% of residents and medical students along with up to 54% of nurses suffer from burnout and work-related stress (4).
Numbers don’t lie – considering the fact that in 2011, the number of burned-out medical staff was 46% (5), the elevated levels are becoming more of an alarming issue now than they were a decade ago.
To understand why the cases are rising, it is important to look at them in the context of change in health systems throughout the years. Because of such pattern change, the aforementioned factors have only intensified.
Factors Influencing Burnout Rates
Society’s increased expectations and updated medical care policies demand more of health care professionals – whether longer working hours, staff shortages, increased administration or intensified workload.
This not only disrupts normal work dynamics but also drives employees to overthink how they intend to improve their performance so as to not fall behind.
On top of that, in less advanced countries, the increase in demand is not supported by the currently available resources. As the population keeps growing and aging, more clinicians and healthcare professionals are needed. That said, one of the main issues for many healthcare disciplines is the limited workforce and staff present. In some countries, the number of professionals per patient admitted is highly concerning.
Fewer people working means more work for those that do.
All these factors disrupt the healthy work-life balance of employees by simply demanding more than what one can handle. Burnout is no longer a shock as most of these overworked clinicians and nurses end up feeling physically and mentally drained.
How did the pandemic impact healthcare workers?
When the Covid-19 pandemic surfaced in 2020, and as the number of deaths and critically ill patients were exponentially rising, we all relied on healthcare workers to offer us help, comfort, and support.
We don’t talk enough about all the challenges clinicians and nurses had to face to adapt quickly and continue to provide the best care to these patients.
Being placed on the frontline of this global health crisis impacted the healthcare system as a whole as well as the mental health of practitioners on an individual scale.
According to recent studies, the overall prevalence of burnout among healthcare workers was 58%. Specifically, 66% of nurses and physicians are reported to have experienced burnout during the pandemic(6).
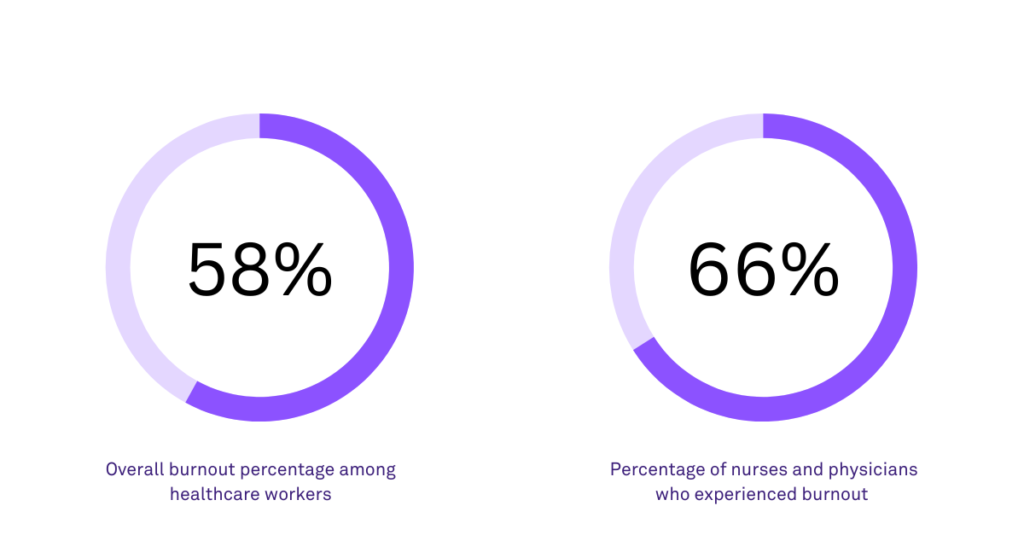
These statistics are not at all surprising.
Not only do these employees have to cope with the high levels of understaffing, uncertainty and limitations in protective equipment, but they also have to manage their fear of getting infected themselves and transmitting the virus to their families.
As with any emergency, we expect front-line healthcare workers to be ready to help, but this time, no precedent was set for dealing with an increase in patient demand in such a short period.
This puts overwhelming pressure on the employees, who are now at higher risk of burnout and psychological stress.
This is reflected by the Physicians Foundation’s 2021 Survey of America’s Physicians (7), the recent study from the International Council of Nurses (8), and other cross-sectional meta-analyses (9,10).
Here are a few alarming statistics from their reports:
- Because of Covid-19, around 57% of physicians had episodes of unexplainable anxiety, anger, and tearfulness.
- During the pandemic, the global rates of burnout among nurses reached a high of 80%.
- 46% of clinicians have experienced isolation or withdrawal from others.
- Compared to 30% in 2020, 34% of physicians experienced an unexplained sense of hopelessness.
- 24.83% and 44.09% of healthcare workers suffered from depression and sleep disorders respectively.
The real issue lies in the fact that professionals in the healthcare sector tend to overlook these mental issues due to a fear of impacting their careers.
Although most of them acknowledge the deterioration in their mental health, only 14% of them actively seek medical attention and professional help (11).
How does burnout affect the workplace and employees? A story from a different perspective.
Compared to the other professions out there, it is clear that physicians, nurses, and other paramedics have at least twice the risk of job burnout.
This undoubtedly results in behavioral dysfunctions and emotional distortions. Burnout tends to negatively manifest itself as feelings of dissatisfaction with work-life balance, exhaustion, and low personal or professional accomplishment.
Let’s look deeper into the different aspects impacted by job burnout in healthcare.
Personal Level
The most apparent consequence of a physician or nurse’s burnout is decreased productivity. Some resort to substance abuse, have negative attitudes towards colleagues, break off relationships, and eventually consider suicide.
The high level of absenteeism experienced by healthcare professionals has caused most of them to call in sick more frequently or retire early. This jeopardizes the continuity of patient management and care.
World health organization (WHO) predicts an increase in hospital staff shortage to reach around 15 million by 2030 (12). Recruitment and staff turnover becomes necessary to fill in the created gaps in productivity.

Organizational/ Patient Level
It is important to point out that when individuals are struggling, the entire system suffers too.
The stakes are higher in healthcare since job performance is closely linked to overall patient satisfaction and quality of care. Medical errors are bound to occur, especially when caregivers are mentally and physically fatigued.
Psychological stress makes you less prone to comply with health and safety regulations which then puts the hospital and employees at risk of falling into legal suits due to malpractice.
What Can Be Done to Fight Employee Burnout?
Reducing work burnout is no easy task. It is clear now that addressing the issue solely at the level of individual clinicians won’t cut it.
The most successful intervention strategy will need to involve both the individual and the institution or organization. Let us start with the most straightforward approaches (13,14).
Employee Based Interventions
A variety of wellness and mindfulness strategies have been tested out throughout the years to help physicians better cope with burnout and improve their work-life balance. The most successful so far have always included some form of cognitive behavioral therapy.
1. Focusing on Improving Relationships
Healing connections is a term first proposed by Dr. Balfour Mount, who along with his colleagues, has noticed isolated and disconnected patients tended to experience higher levels of anguish, despair, and suffering (15).
Considering how most burnout patients also live in hopelessness and distress, it would be safe to assume that healthier relationships with their inner self and the people around them will generate healing in a sense.
Hence why physicians and nurses should prioritize spending more time with family, significant others, and friends outside of the workplace. And during work hours, it may be a good idea to generate healthy bonds with fellow staff members and colleagues.
Heal those broken connections and maintain inner and outer peace through solid relationships.
2. Mindfulness and Self-care Activities
Self-awareness is the first step toward fixing the problem. Once you identify the source of the burnout, it is then important to invest time in seeking practices that reduce or eliminate it. It isn’t complicated; these practices could be as simple as everyday activities or small changes in your daily routine. Gaining mental clarity should be a priority for everyone working in high pressure environments.
Get more sleep, eat better, exercise, and if you feel like you can’t handle the physical or psychological burden, seek professional counseling.
A very robust and protocolized intervention gaining attention is “Mindfulness-Based Stress Reduction”. As the name entails, this strategy is 8 weekly sessions all about stress relieving techniques and mindfulness training.
By enabling perspective-taking, this technique helps in building new healthy ways of perceiving anxiety situations. The data on Mindfulness-Based Stress Reduction support the benefits gained in terms of burnout prevention and reduction (16).
Organization Based Interventions
To support optimal well-being among work staff, the organization or institution has to play its role right by first recognizing the presence of a problem and developing a strategy of its own to create a supportive and healthier work environment.
Slutions could involve providing more work autonomy and control, ensuring more flexible schedules, and breaking the stigmatizations around mental health. Interventions such as Resilience Institute Precision Training demonstrate consistent and dramatic shifts in organizational resilience, including amongst healthcare workers.
In 2017, Shanafelt and Noseworthy have designed an evidence-based, 9-step intervention to help organizations reduce the levels of burnout of employees (17). To summarize them:
1. Putting effort into regularly measuring staff well-being to acknowledge and assess burnout as a real problem. There are a lot of self-assessing applications that help you measure your resilience ratio score and provide you with tips to improve your lifestyle accordingly.
2. Reduce the level of toxic work relationships by promoting healthy leadership behavior.
3. Make system improvements and interventions less general and more targeted to the actual problem detected. Sometimes, maximum local impact in each department is most effective.
4. Provide support by promoting positive and constructive discussions and cultivating a healthy community at work.
5. Wisely use rewards and incentives that drive employees to collectively work towards a common goal.
6. Better align the organization’s values with a healthy and collaborative work culture.
7. Enhance work-life balance by promoting flexible and family-friendly environments at work.
8. Offer the opportunity to promote self-care and provide activities that improve mental fitness, emotion regulation and resilience.
9. Generate robust, evidence-based scientific discoveries by facilitating and funding science within the organization. Discoveries can then be implemented within the institution to enhance staff engagement and reduce burnout.
10. The final step, is to assist any colleague who is suffering from burnout and ensuring they reintegrate the workplace with a healthy mindset. By following these steps, you are sure that post burnout, your employees return to work in a proper way.
Summary
Burnout in healthcare systems is a serious concern. When caregivers are burned out, their well-being is not the only thing suffering. Those impacted include colleagues, family members, and friends but mostly patients.
Developing individual and organizational resilience strategies is a step in the right direction. Leaders should model and implement daily rhythms that deliver performance with care.
Burnout – physical, emotional and mental distress – drains vitality, but consistent self-care, mindfulness, and the right work environment enable rapid bounce.
Sources:
1. Depression: What is burnout? [Internet]. InformedHealth.org [Internet]. Institute for Quality and Efficiency in Health Care (IQWiG); 2020 [cited 2022 Oct 14]. Available from: https://www.ncbi.nlm.nih.gov/books/NBK279286/
2. ICD-11 for Mortality and Morbidity Statistics [Internet]. [cited 2022 Oct 14]. Available from: https://icd.who.int/browse11/l-m/en#/http://id.who.int/icd/entity/129180281
3. Lucas G, Colson S, Boyer L, Inthavong K, Haller PH, Lancon C, et al. Risk factors for burnout and depression in healthcare workers: The national AMADEUS study protocol. L’Encéphale. 2022 Jun 1;48(3):247–53.
4. Committee on Systems Approaches to Improve Patient Care by Supporting Clinician Well-Being, National Academy of Medicine, National Academies of Sciences, Engineering, and Medicine. Taking Action Against Clinician Burnout: A Systems Approach to Professional Well-Being [Internet]. Washington, D.C.: National Academies Press; 2019 [cited 2022 Oct 14]. Available from: https://www.nap.edu/catalog/25521
5. Shanafelt TD, Hasan O, Dyrbye LN, Sinsky C, Satele D, Sloan J, et al. Changes in Burnout and Satisfaction With Work-Life Balance in Physicians and the General US Working Population Between 2011 and 2014. Mayo Clin Proc. 2015 Dec;90(12):1600–13.
6. Ghahramani S, Lankarani KB, Yousefi M, Heydari K, Shahabi S, Azmand S. A Systematic Review and Meta-Analysis of Burnout Among Healthcare Workers During COVID-19. Front Psychiatry. 2021 Nov 10;12:758849.
7. The Physicians Foundation 2021 Physician Survey: COVID-19 Impact Edition: A Year Later [Internet]. The Physicians Foundation. [cited 2022 Oct 14]. Available from: https://physiciansfoundation.org/physician-and-patient-surveys/the-physicians-foundation-2021-physician-survey/
8. The COVID-19 Effect: World’s nurses facing mass trauma, an immediate danger to the profession and future of our health systems [Internet]. ICN – International Council of Nurses. [cited 2022 Oct 14]. Available from: https://www.icn.ch/news/covid-19-effect-worlds-nurses-facing-mass-trauma-immediate-danger-profession-and-future-our
9. Marvaldi M, Mallet J, Dubertret C, Moro MR, Guessoum SB. Anxiety, depression, trauma-related, and sleep disorders among healthcare workers during the COVID-19 pandemic: A systematic review and meta-analysis. Neurosci Biobehav Rev. 2021 Jul 1;126:252–64.
10. Sahebi A, Nejati-Zarnaqi B, Moayedi S, Yousefi K, Torres M, Golitaleb M. The prevalence of anxiety and depression among healthcare workers during the COVID-19 pandemic: An umbrella review of meta-analyses. Prog Neuropsychopharmacol Biol Psychiatry. 2021 Apr 20;107:110247.
11. Leo CG, Sabina S, Tumolo MR, Bodini A, Ponzini G, Sabato E, et al. Burnout Among Healthcare Workers in the COVID 19 Era: A Review of the Existing Literature. Front Public Health [Internet]. 2021 [cited 2022 Oct 14];9. Available from: https://www.frontiersin.org/articles/10.3389/fpubh.2021.750529
12. Health workforce [Internet]. [cited 2022 Oct 14]. Available from: https://www.who.int/health-topics/health-workforce
13. McFarland DC, Hlubocky F. Therapeutic Strategies to Tackle Burnout and Emotional Exhaustion in Frontline Medical Staff: Narrative Review. Psychol Res Behav Manag. 2021 Sep 15;14:1429–36.
14. De Hert S. Burnout in Healthcare Workers: Prevalence, Impact and Preventative Strategies. Local Reg Anesth. 2020 Oct 28;13:171–83.
15. Mount BM, Boston PH, Cohen SR. Healing Connections: On Moving from Suffering to a Sense of Well-Being. J Pain Symptom Manage. 2007 Apr 1;33(4):372–88.
16. Kriakous SA, Elliott KA, Lamers C, Owen R. The Effectiveness of Mindfulness-Based Stress Reduction on the Psychological Functioning of Healthcare Professionals: a Systematic Review. Mindfulness. 2021;12(1):1–28.
17. Shanafelt TD, Noseworthy JH. Executive Leadership and Physician Well-being: Nine Organizational Strategies to Promote Engagement and Reduce Burnout. Mayo Clin Proc. 2017 Jan 1;92(1):129–46.

